Kisspeptin: Restoring Testosterone and Hormonal Balance
Discover how kisspeptin restores testosterone & hormonal balance by activating the HPG axis. Learn the research, benefits, dosing, and sourcing guide for 2026.
What if one small peptide could flip the switch on your entire hormonal system?
That is exactly what kisspeptin does. It sits at the top of the hormonal command chain, acting as the master signal that tells your brain to start producing testosterone and other sex hormones. Without kisspeptin doing its job, the entire system can fall silent.
For researchers studying hypogonadism, fertility challenges, and hormonal imbalances, kisspeptin has quickly become one of the most exciting compounds in modern endocrinology. Unlike synthetic testosterone that replaces hormones from the outside in, kisspeptin works from the inside out by waking up the brain's own hormone-producing machinery.
This guide breaks down exactly how kisspeptin works, what the research shows, and why scientists around the world are studying it as a potential solution for hormone deficiency. If you are new to peptide research, our Complete Beginner's Guide to Peptide Therapy is a great place to start.
What Is Kisspeptin? The Hormone Gatekeeper
Kisspeptin is a neuropeptide, meaning it is a small protein-like molecule that sends signals between nerve cells in the brain. It was first discovered in 1996 and originally named metastin because of its ability to suppress cancer metastasis. But researchers quickly realized it had an even bigger role to play in the hormonal system.
The name kisspeptin comes from Hershey, Pennsylvania, the home of Hershey's Kisses chocolate and where many of the early kisspeptin discoveries were made. It is a fun fact that tends to stick.
Kisspeptin is produced mainly in a small area of the brain called the hypothalamus. Specifically, it is made by neurons in two regions called the arcuate nucleus and the anteroventral periventricular nucleus (AVPV). These neurons are sometimes called KNDy neurons because they also produce two other signaling molecules, neurokinin B and dynorphin, that work alongside kisspeptin.
The Master Switch for Hormone Production
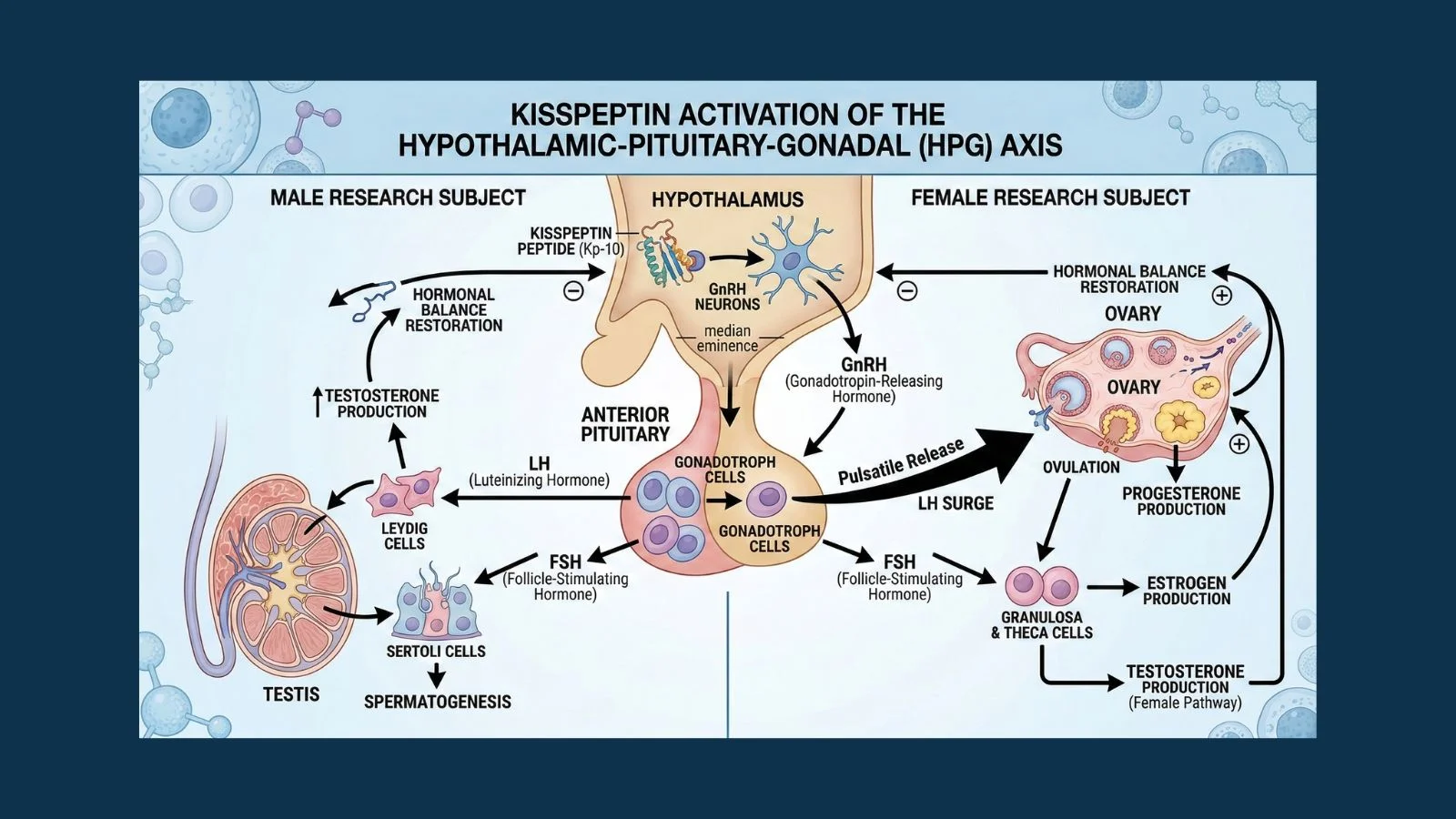
Here is where kisspeptin becomes truly remarkable. When kisspeptin is released, it binds to a receptor on the surface of other neurons called KISS1R (also known as GPR54). This triggers those neurons to release a hormone called gonadotropin-releasing hormone, or GnRH.
GnRH then travels to the pituitary gland, which sits just below the hypothalamus. The pituitary responds by releasing two more hormones: luteinizing hormone (LH) and follicle-stimulating hormone (FSH).
LH travels through the bloodstream to the gonads. In men, LH signals the testes to produce testosterone. In women, LH triggers ovulation and signals the ovaries to produce estrogen and progesterone.
This entire chain is called the hypothalamic-pituitary-gonadal (HPG) axis. Kisspeptin is the first link in that chain. Without it, the whole system stalls.
Research published in PMC (PubMed Central) confirms that kisspeptin neurons are the primary drivers of GnRH pulsatility, the rhythmic bursts of GnRH that keep hormones balanced and fertile cycles running properly.
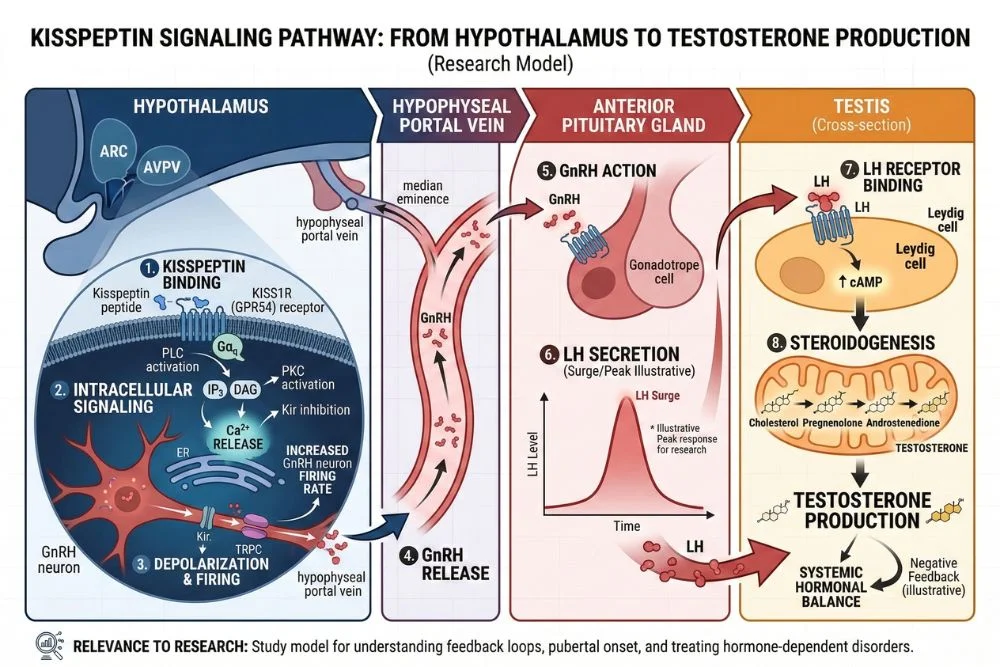
How Kisspeptin Works: The Step-by-Step Pathway
Understanding the kisspeptin pathway is like learning how a domino chain works. Each piece triggers the next. Here is how it unfolds from start to finish.
Step 1: Kisspeptin Is Released in Pulses
Kisspeptin is not released in one steady stream. It fires in pulses, which is critically important. The pituitary gland and gonads respond best to rhythmic signals, not constant ones. A steady, non-pulsatile signal actually causes the system to shut down, a concept called receptor desensitization.
This is one of the key reasons kisspeptin is so exciting for research. Unlike continuous GnRH analogs that can suppress hormone production over time, pulsatile kisspeptin administration mirrors the body's natural rhythm.
Step 2: KISS1R Activation Triggers GnRH
When kisspeptin binds to the KISS1R receptor on GnRH neurons, it activates a cascade inside the cell. Calcium levels rise, which causes the neuron to fire and release GnRH into the bloodstream in small bursts.
A landmark study in the New England Journal of Medicine showed that when participants with hypogonadotropic hypogonadism received kisspeptin injections, their LH and FSH levels rose significantly, confirming that the pathway was being activated in real human subjects.
Step 3: LH Surge and Testosterone Production
Once GnRH reaches the pituitary, LH is released in a corresponding pulse. In men, each LH pulse signals the Leydig cells in the testes to produce testosterone. More frequent and robust LH pulses generally result in higher circulating testosterone levels.
In women, LH pulses regulate the menstrual cycle. The largest LH surge of the month triggers ovulation, the release of an egg from the ovary. Kisspeptin is directly responsible for generating this surge.
Step 4: Negative Feedback Keeps Things Balanced
Once testosterone and estrogen levels rise, they feed back to the hypothalamus and pituitary, telling the system to slow down kisspeptin production. This built-in feedback loop is what keeps hormones in balance rather than spiraling out of control.
It is a beautifully self-regulating system, and kisspeptin is the conductor that keeps everything in rhythm.
What Happens When Kisspeptin Levels Are Low?
When kisspeptin signaling is disrupted, the downstream effects are significant. Because kisspeptin sits at the very top of the HPG axis, low kisspeptin levels can cause a condition called hypogonadotropic hypogonadism (HH), where the brain simply does not send enough signal to the gonads to produce hormones.
This is different from primary hypogonadism, where the gonads themselves are damaged. In hypogonadotropic hypogonadism, the gonads are healthy but not receiving proper instructions. The problem is upstream, in the brain's signaling network.
Causes of Low Kisspeptin Activity
Several factors can reduce kisspeptin signaling:
- Genetic mutations in the KISS1 or KISS1R genes (Kallmann syndrome and similar conditions)
- Chronic stress, which elevates cortisol and suppresses kisspeptin neurons
- Extreme caloric restriction or low body fat, which is why elite athletes and people with eating disorders often lose their reproductive hormones
- Aging, since kisspeptin neuron activity naturally declines with age
- Certain medications and environmental estrogens that disrupt hypothalamic signaling
Symptoms of Reduced Kisspeptin Signaling
In men, low kisspeptin activity can produce symptoms such as low testosterone, reduced libido, fatigue, mood disruption, poor sleep quality, reduced muscle mass, and infertility. In women, it can cause absent or irregular periods, low estrogen, hot flashes, and infertility.
Research in PMC Endocrinology confirms that mutations in the KISS1R gene are directly linked to conditions of delayed puberty and reproductive failure, underlining how essential this peptide is for normal hormonal development.
The Research Case for Kisspeptin
Over the past two decades, kisspeptin has moved from an obscure cancer research finding to one of the most studied compounds in reproductive endocrinology. The research is compelling, and the implications go well beyond fertility.
Kisspeptin and Male Hypogonadism
One of the most promising research areas is using kisspeptin to restore testosterone in men with hypogonadotropic hypogonadism. Standard testosterone replacement therapy (TRT) works by adding testosterone from the outside, but it also suppresses the body's own production and can reduce sperm count to zero.
Kisspeptin offers a different approach. By stimulating the brain's own GnRH neurons, it encourages the body's natural testosterone production to restart without shutting down the reproductive system. This is especially important for men who want to maintain fertility while also restoring their testosterone levels.
Kisspeptin and Female Fertility
In women, kisspeptin research has focused heavily on triggering ovulation. In conventional IVF protocols, a synthetic hormone called hCG is used to trigger egg release. But hCG carries a risk of a dangerous complication called ovarian hyperstimulation syndrome (OHSS).
Researchers discovered that kisspeptin can trigger the LH surge needed for ovulation through a completely natural pathway, potentially reducing OHSS risk dramatically.
A groundbreaking study published in The Lancet showed that kisspeptin successfully triggered ovulation in IVF patients at high risk for OHSS, with no serious complications reported, opening a new chapter in fertility medicine.
Kisspeptin and Puberty Research
Kisspeptin is also being studied for its role in triggering puberty. In children with constitutional delay of puberty or genetic conditions like Kallmann syndrome, kisspeptin may offer a way to activate the HPG axis and initiate normal hormonal development.
Animal models have shown that kisspeptin administration can advance puberty onset, and early human studies are exploring similar approaches for clinical application.
Kisspeptin and Metabolic Health
The reach of kisspeptin research extends into metabolic science. Kisspeptin receptors have been found in tissues beyond the hypothalamus, including the pancreas, liver, and adipose tissue, hinting that kisspeptin may play a broader role in metabolism than previously understood.
Research from PubMed suggests kisspeptin may influence insulin secretion and glucose metabolism, which could eventually connect kisspeptin research to the broader world of metabolic optimization. For more on how peptides influence metabolism, see our guide on Peptides for Fat Loss.
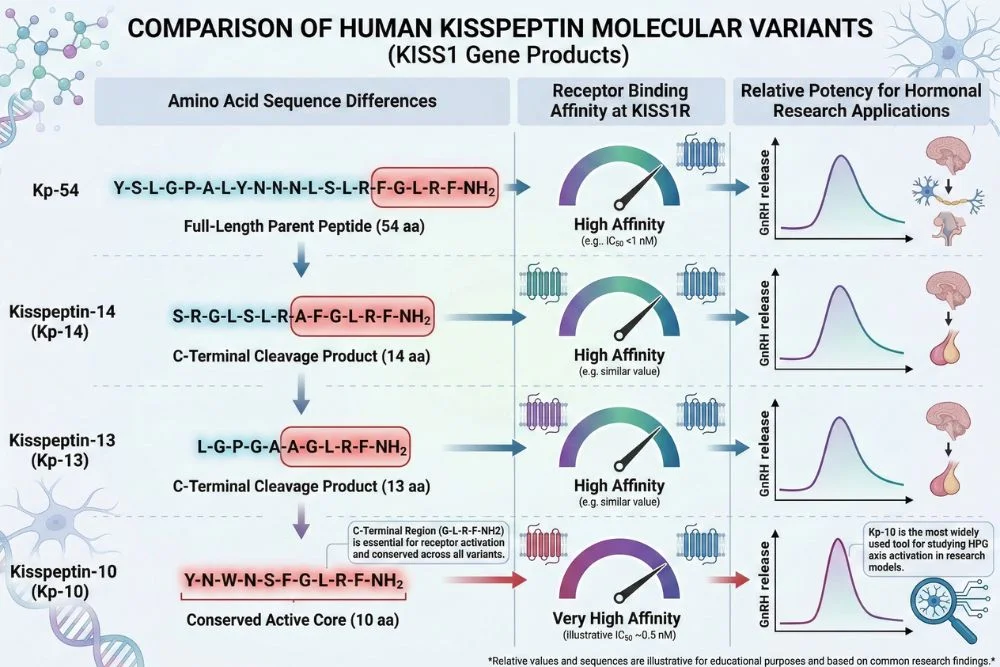
Kisspeptin Variants: What Forms Are Being Studied?
Kisspeptin is not a single molecule. It exists in several forms, each with slightly different potencies and durations of action.
Kisspeptin-54 (Metastin 45-54)
Kisspeptin-54 is the full-length form of the peptide, containing 54 amino acids. It is the primary circulating form in humans and the version most commonly used in clinical research. It has a relatively short half-life of around 28 minutes when administered intravenously.
Kisspeptin-10
Kisspeptin-10 contains just 10 amino acids but retains full binding activity at the KISS1R receptor. It is the most studied fragment in research settings because it is easier to synthesize, more stable, and nearly as potent as the full-length version. Most modern kisspeptin research uses kisspeptin-10.
Kisspeptin-13 and Kisspeptin-14
These intermediate fragments are less commonly used but have shown activity in animal models. Kisspeptin-14 is the primary form found in sheep, which has made it useful in reproductive research with livestock.
For research purposes, kisspeptin-10 is the most widely available and most studied form, offering a practical balance of potency, stability, and synthesizability.
Research Protocols and Dosing Considerations
Important note: The following information is based on published research studies conducted by licensed researchers in controlled clinical and laboratory settings. Kisspeptin is a research peptide and is not approved for human use outside of clinical trials. This section is for educational purposes only.
Kisspeptin-10 Research Protocols
In published studies, kisspeptin-10 has been administered through several routes depending on the research objective:
- Intravenous (IV) infusion: Used in acute studies measuring immediate LH and testosterone response, typically at doses ranging from 0.1 to 4 nanomoles per kilogram of body weight
- Subcutaneous (SC) injection: Used in longer-duration studies, with doses typically in the range of 1 to 10 micrograms per kilogram
- Intranasal delivery: Being explored for convenience and non-invasive administration
Research timing matters significantly with kisspeptin because of the pulsatile nature of GnRH signaling. Studies have used single-pulse, multi-pulse, and continuous infusion protocols, with pulsatile protocols generally producing more sustained hormonal responses.
Reconstitution and Storage
Kisspeptin peptides are typically supplied as lyophilized (freeze-dried) powder. For research use, they are reconstituted with bacteriostatic water. Once reconstituted, solutions should be stored at 4 degrees Celsius and used within a short window to maintain peptide stability.
To calculate precise research amounts, the Peptide Calculator Guide walks through the exact steps for reconstitution and dosing accuracy.
Interpreting Research Data
Published studies consistently show that kisspeptin administration produces a measurable LH response within 30 to 60 minutes, followed by a testosterone rise that peaks at 60 to 120 minutes. The magnitude of response appears to depend on baseline hormonal status, kisspeptin dose, and the pulse frequency used.
Kisspeptin and Testosterone: Key Research Findings
The connection between kisspeptin and testosterone is now well-established. Here is a summary of what the research shows.
Direct Testosterone Stimulation
Multiple studies confirm that kisspeptin administration reliably increases LH and subsequently testosterone in healthy men and men with hypogonadotropic hypogonadism. The effect is dose-dependent and consistent across different kisspeptin variants.
What makes this significant is that the testosterone response comes through the body's own HPG axis, not from exogenous hormones. This means testicular function is preserved, and sperm production is not suppressed as it would be with standard TRT.
Restoring the HPG Axis After Suppression
One intriguing research area involves using kisspeptin to help restart the HPG axis in men who have been on anabolic steroids or testosterone therapy, which suppress natural production. Because kisspeptin acts at the very top of the signaling chain, it may offer a pathway to restore natural hormone production even when the axis has been suppressed for extended periods.
This is still an active area of research, but early findings are encouraging. Animal models have shown successful HPG axis reactivation following kisspeptin administration after prolonged suppression.
Testosterone and Mood Regulation
Testosterone plays an important role in mood, motivation, and cognitive function. Because kisspeptin drives testosterone through the natural pathway, researchers are also exploring its potential connection to mood disorders related to hormonal decline.
Interestingly, kisspeptin neurons themselves have connections to brain regions involved in emotion and reward, suggesting kisspeptin may have direct neurological effects beyond its hormonal role. Some early research has even explored kisspeptin as a potential tool in the study of sexual motivation and bonding behaviors.
How Kisspeptin Compares to Other Hormonal Research Peptides
Kisspeptin occupies a unique space in peptide research because it targets the very beginning of the hormonal cascade rather than downstream effects.
Kisspeptin vs. hCG
Human chorionic gonadotropin (hCG) mimics LH and directly stimulates the testes to produce testosterone. It works, but it bypasses the brain entirely and can cause receptor desensitization over time with chronic use. Kisspeptin, by contrast, works through the brain's own GnRH neurons, producing a more physiologically normal hormone pattern.
Kisspeptin vs. Clomiphene
Clomiphene (Clomid) is a selective estrogen receptor modulator that reduces estrogen feedback, causing the hypothalamus to increase GnRH output. It increases LH and testosterone indirectly. Kisspeptin takes a more direct route by activating GnRH neurons through a dedicated receptor. Research suggests kisspeptin produces a stronger and more targeted LH pulse than clomiphene.
Kisspeptin vs. Gonadorelin
Gonadorelin is a synthetic GnRH analog used to stimulate LH directly from the pituitary. Kisspeptin is one step upstream from GnRH, meaning it allows the full natural signal to develop before reaching the pituitary. This upstream position may offer advantages in terms of maintaining normal GnRH neuron health and activity over time.
For a broader look at how different peptide compounds interact with the endocrine system, our guide on Peptide Therapy Basics provides helpful context.
Safety Profile and Considerations in Research
Kisspeptin has shown a favorable safety profile in clinical research to date. Here is what the published data indicates.
Reported Side Effects in Clinical Studies
In human clinical trials, kisspeptin has generally been well-tolerated. The most commonly reported effects include temporary flushing at the injection site, mild nausea in some subjects, and transient increases in blood pressure in a small number of cases. No serious adverse events directly attributable to kisspeptin have been reported in published studies.
Tachyphylaxis and Receptor Desensitization
One important research consideration is receptor desensitization. If kisspeptin is administered continuously rather than in pulses, the KISS1R receptor can become desensitized, leading to reduced response over time. This is why pulsatile protocols are preferred in research settings and why dosing frequency matters.
Potential for Hormonal Overstimulation
Because kisspeptin activates the full HPG axis, there is a theoretical risk of hormonal overstimulation if doses are too high or administered too frequently. In clinical studies, this has been managed through careful dose titration and monitoring.
All kisspeptin research should be conducted by qualified professionals in properly equipped laboratory settings with appropriate monitoring and ethical oversight.
Sourcing Quality Kisspeptin for Research
As with all research peptides, quality matters enormously when sourcing kisspeptin. Impure or incorrectly synthesized peptides can produce unreliable data and unexpected effects.
What to Look for in a Research Supplier
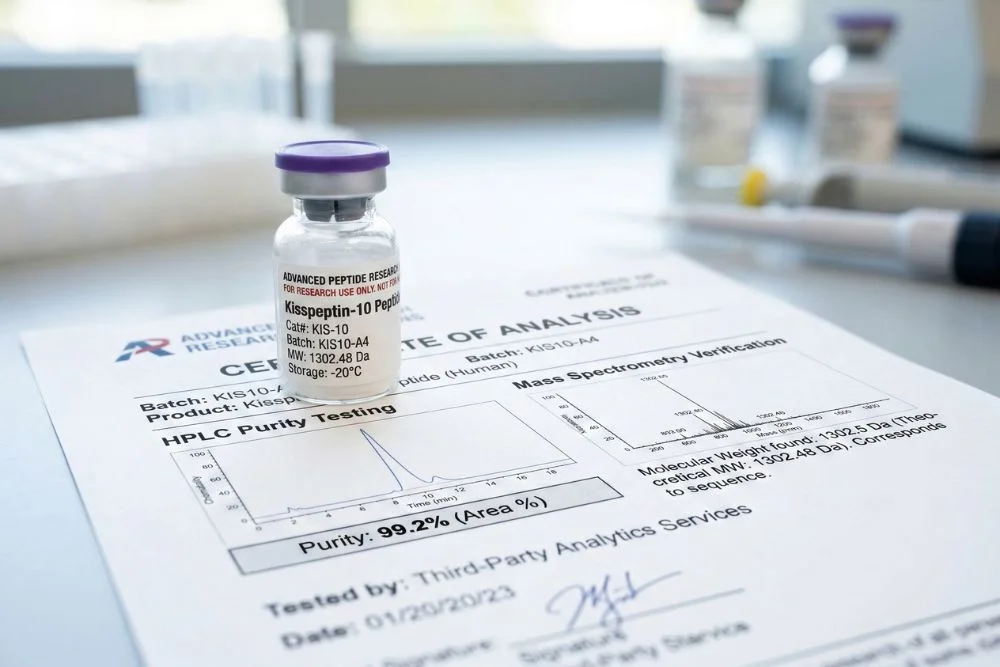
Look for suppliers who provide a Certificate of Analysis (CoA) from a third-party laboratory for every batch. The CoA should confirm peptide purity (ideally above 98%), molecular weight, and amino acid sequence verification.
Not sure how to read a Certificate of Analysis? Our detailed guide on How to Read a Peptide Certificate of Analysis explains exactly what to look for before purchasing any research compound.
Red Flags to Avoid
- No CoA available or only in-house testing with no third-party verification
- Unusually low prices that suggest corner-cutting in synthesis or testing
- No clear labeling of peptide form (kisspeptin-10 vs. kisspeptin-54)
- Suppliers who make medical claims or market as human supplements
Recommended Supplier
For verified kisspeptin research peptides, Peptides Finder connects researchers with vetted suppliers who provide full third-party testing documentation.
Browse Kisspeptin Research Compounds at Peptides Finder
We may earn a commission from purchases made through links on this page.
Frequently Asked Questions
What is kisspeptin and what does it do?
Kisspeptin is a neuropeptide produced in the hypothalamus that acts as the master switch for the hormonal system. It binds to the KISS1R receptor on GnRH neurons, triggering the release of gonadotropin-releasing hormone. This starts a cascade that leads to LH and FSH release from the pituitary, and ultimately testosterone production in men or ovulation and estrogen production in women. Without adequate kisspeptin signaling, the entire reproductive hormone axis can fall dormant, which is why it is such an important research target.
How does kisspeptin increase testosterone?
Kisspeptin increases testosterone by activating the HPG axis from the top down. When kisspeptin fires in pulses, it causes GnRH neurons to release GnRH. GnRH then stimulates the pituitary to release LH. LH travels to the testes and signals the Leydig cells to produce testosterone. This is the body's own natural pathway for testosterone production, which is why kisspeptin is considered a more physiologically normal approach compared to direct testosterone replacement.
What is the difference between kisspeptin-10 and kisspeptin-54?
Kisspeptin-54 is the full-length form of the peptide, containing 54 amino acids. It is the primary form circulating in the human body. Kisspeptin-10 is a shorter fragment of just 10 amino acids that retains full activity at the KISS1R receptor. Kisspeptin-10 is more commonly used in research because it is easier and less expensive to synthesize, more stable in solution, and produces nearly identical receptor activation compared to the full-length version.
Can kisspeptin be used for fertility treatment?
Clinical research has explored kisspeptin as a trigger for ovulation in IVF protocols. A landmark study published in The Lancet showed kisspeptin successfully triggered ovulation in women at high risk for ovarian hyperstimulation syndrome (OHSS), a dangerous complication associated with conventional hCG triggers. By using the body's own LH surge mechanism instead of synthetic hCG, kisspeptin may offer a safer option for certain fertility patients. However, this remains an area of ongoing research and is not yet approved as a standard clinical treatment.
What happens if kisspeptin levels are too low?
Low kisspeptin levels or mutations in the KISS1 or KISS1R genes can cause hypogonadotropic hypogonadism, a condition where the brain does not produce enough GnRH to drive hormonal production. In men, this leads to low testosterone, low sperm count, reduced libido, fatigue, and mood changes. In women, it causes absent or irregular periods, low estrogen, and infertility. Kisspeptin deficiency can also be acquired through chronic stress, extreme dieting, or certain medications that suppress hypothalamic signaling.
Is kisspeptin safe for research?
In published clinical trials, kisspeptin has demonstrated a favorable safety profile with no serious adverse events directly attributable to its administration. Common observations have included mild injection site reactions and occasional transient flushing. The main research concern is receptor desensitization if kisspeptin is administered in a continuous rather than pulsatile manner. All research involving kisspeptin should be conducted by qualified professionals in controlled laboratory environments with appropriate monitoring protocols in place.
How is kisspeptin different from testosterone replacement therapy?
Testosterone replacement therapy (TRT) provides testosterone from an external source, which signals the body to stop its own production. This suppresses LH, FSH, and natural testosterone synthesis, and can reduce sperm count to near zero. Kisspeptin takes the opposite approach by stimulating the brain to restart its own hormonal cascade. This preserves testicular function and sperm production, making it particularly relevant for research into male fertility alongside hormonal restoration. It is a fundamentally different mechanism with different implications for the reproductive system.
Conclusion: Kisspeptin as the Future of Hormonal Research
Kisspeptin represents something rare in peptide science: a single compound that controls the entire hormonal axis from its origin point. By targeting GnRH neurons directly, it offers researchers a way to study hormonal restoration, fertility activation, and HPG axis function in a way that mirrors the body's own biology far more closely than existing pharmaceutical options.
The research continues to build momentum. From clinical trials in hypogonadotropic hypogonadism to IVF ovulation triggering, from puberty research to metabolic connections, kisspeptin is proving to be one of the most versatile and impactful research compounds in modern endocrinology.
For researchers interested in hormonal balance, reproductive health, and the neuroscience of the HPG axis, kisspeptin belongs at the center of the conversation. As science advances, the applications of kisspeptin research will only continue to expand.
Explore our full library of peptide research guides at Peptides Finder, and stay ahead of the latest developments in hormonal science.
Official Research Disclaimer
The information provided in this guide is for informational and educational purposes only. Kisspeptin is sold as a research chemical. Research peptides are intended strictly for laboratory research and are not for human consumption or for the diagnosis, treatment, or prevention of any disease. All research should be conducted by qualified professionals in controlled environments with proper ethical oversight. This article does not constitute medical advice. Always consult a licensed healthcare provider before using any research compound. Never disregard professional medical advice or delay seeking it because of information you read online. The author and publisher disclaim any liability for adverse effects resulting from the use or application of the information contained herein.