
The History of GLP-1: From Discovery to Therapeutics
We explore the fascinating history of Glucagon-Like Peptide-1 (GLP-1), the accidental discoveries, and the scientists who changed metabolic medicine.
In 2026, glucagon-like peptide-1 (GLP-1) is arguably the most famous molecule in the world. It has upended the food industry, reshaped the stock market, and changed how we define obesity.
But this "overnight success" was actually 40 years in the making.
The story of how we harnessed this hormone is not a straight line. It involves a rejected research paper, a venomous lizard from the American Southwest, and a decades-long battle against a microscopic enzyme that destroys the molecule before it can work.
To understand the future of weight loss, we must look back at the incredible scientific detective story that brought us here.
1980s: The "Incidental" Discovery
In the early 1980s, researchers were not looking for a weight loss drug. They were studying the pancreas to understand diabetes.
Scientists knew that the proglucagon gene produced glucagon (which raises blood sugar). But when they sequenced the gene, they found something odd: two other peptide sequences hidden inside the genetic code. They named them Glucagon-Like Peptide-1 and Glucagon-Like Peptide-2.
Initial excitement faded quickly. When researchers injected natural GLP-1 into humans, it worked perfectly to lower blood sugar... for about 90 seconds.
The problem was an enzyme called DPP-4 (Dipeptidyl Peptidase-4). As we discussed in our article on What Is Glucagon-Like Peptide-1?, this enzyme acts like a shredder, destroying the hormone almost instantly. As a drug, natural GLP-1 was useless.
1992: The Lizard in the Lab
The breakthrough came from an unlikely source: the Bronx VA Hospital in New York. Dr. John Eng was studying the venom of the Gila Monster (Heloderma suspectum), a sluggish lizard known to maintain stable blood sugar even when it didn't eat for months.
Dr. Eng discovered a peptide in the venom that was remarkably similar to human GLP-1, but with one crucial difference: it was immune to the DPP-4 enzyme. He named it Exendin-4.
According to his seminal paper published in the Journal of Biological Chemistry, this lizard peptide could remain active in the bloodstream for hours, not minutes. It was the "stable" version of the hormone scientists had been dreaming of.
Incredibly, major pharmaceutical companies initially rejected Dr. Eng's discovery. It wasn't until 2005 that the first drug based on this venom, Exenatide (Byetta), was approved by the FDA for Type 2 Diabetes.
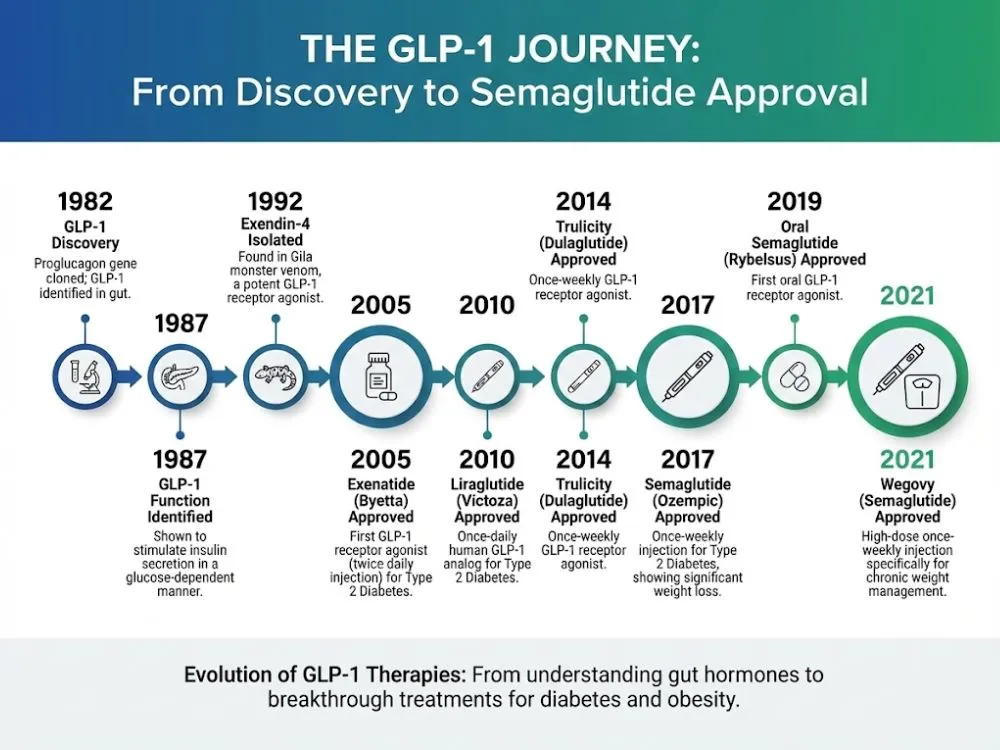
2010: The Liraglutide Era
While lizard venom worked, the pharmaceutical race was on to create a human analog, a synthetic version of the hormone that looked like ours but resisted degradation.
This led to the development of Liraglutide (Victoza/Saxenda). By attaching a fatty acid chain to the peptide, scientists allowed it to bind to albumin in the blood, protecting it from enzymes and extending its half-life to roughly 13 hours.
This was a massive leap forward. Patients no longer needed twice-daily injections; they could inject once a day.
But more importantly, researchers noticed a side effect: the patients weren't just controlling their blood sugar, they were losing significant weight.
A comprehensive review in Therapeutics and Clinical Risk Management details how this discovery shifted the entire focus of glucagon-like peptide-1 research from diabetes management to obesity treatment.
2017–Present: The Semaglutide Revolution
The game changed forever with the introduction of Semaglutide (Ozempic/Wegovy).
Through precise chemical engineering, scientists tweaked the molecule to survive in the body for a full week. As detailed in our breakdown of GLP-1 Drugs Explained, this weekly dosing schedule solved the biggest hurdle in peptide therapy: patient compliance.
The results were undeniable. In the famous "STEP 1" clinical trials published in the New England Journal of Medicine (NEJM), patients achieved weight loss numbers that had previously only been seen with bariatric surgery.
The era of medical weight management had officially begun.
The Future: Beyond the Needle
The history of GLP-1 is still being written. The next chapter involves "Oral GLP-1s" (pills) and "Dual/Triple Agonists" (like Retatrutide) that target multiple hormone receptors simultaneously.
What started as a biological curiosity in a gene sequence has evolved into a therapeutic class that may eventually treat addiction, Alzheimer's, and heart disease. It serves as a reminder that in science, the most powerful cures often come from the places we least expect, even the saliva of a desert lizard.
Frequently Asked Questions
Who discovered GLP-1?
The specific gene sequence was identified in the early 1980s by varying teams, including Joel Habener at Massachusetts General Hospital and Jens Juul Holst in Copenhagen.
However, Dr. John Eng is credited with discovering Exendin-4 (the lizard venom analog) which made the first drug possible.
Why did early GLP-1 experiments fail?
Because of the enzyme DPP-4. In early human trials, injected natural GLP-1 was destroyed by the body in less than 2 minutes, meaning it had no lasting therapeutic effect until synthetic versions were engineered.
Is Ozempic made from lizard venom?
No. The first drug, Exenatide (Byetta), was a synthetic copy of Gila Monster venom.
Modern drugs like Ozempic (Semaglutide) are 94% homologous to human GLP-1, engineered in a lab to be long-lasting.
When was GLP-1 approved for weight loss?
While it was used for diabetes since 2005, the FDA specifically approved Liraglutide (Saxenda) for weight management in 2014.
Semaglutide (Wegovy) followed in 2021, marking the start of the current boom.
Are there natural sources of GLP-1?
You cannot eat GLP-1 directly, but you can eat foods that stimulate your body to make it.
As we explain in What Are Peptides?, nutrients like fiber and protein trigger the L-cells in your gut to release your own natural reserves.
Conclusion
The history of glucagon-like peptide-1 is a testament to perseverance. It took forty years to turn a fleeting biological signal into a life-saving therapy.
As we stand on the brink of new discoveries in 2026, we are finally realizing the full potential of the body's own satiety system.
Official Medical Disclaimer
The information provided in this guide is for informational and educational purposes only.
Peptides and GLP-1 research compounds are intended strictly for laboratory research and are not for human consumption or for the diagnosis, treatment, or prevention of any disease. All research should be conducted by qualified professionals in a controlled environment. The statements regarding these products have not been evaluated by the Food and Drug Administration (FDA). Always consult your local laws and institutional guidelines regarding the use of peptides in research. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.